Community service for health professionals to improve services
By Salah Elzein Mohamed
South Africa is implementing community service for health professionals as a strategy to cope with the problems of human resources in the health sector. The government hopes that this strategy will ensure improved provision of health services to all citizens of the country. So far, almost 13 000 young health professionals have performed community service at public health facilities in the nine provinces, the South African Military Health Services and the Department of Correctional Services.
The one-year period of community service for health professionals has been implemented in South Africa since 1998. The first group to be deployed for a 12-month period of service in public health facilities comprised the young doctors in 1999, followed by the dentists in 2000 and the pharmacists in 2001. A further seven professional groups followed in 2003, including physiotherapists, occupational and speech therapists, clinical psychologists, dieticians, radiographers and environmental health officers. In 2004, the Health Minister announced that community service will be extended to include nurses once the Nursing Bill has been passed by Parliament.
Health Department places professionals
The national Department of Health is responsible for the placement of the health professionals into posts in the different provinces. The placement process is finalised by September each year to ensure that graduates have certainty about where they will take up their posts during the next year. According to the Health Systems Trust (www.hst.org.za/healthstats), 7 166 health professionals (5 518 doctors, 1 231 pharmacists and 417 dentists) had completed their community service by the end of 2003. The table below details the numbers of each group by year.
Number of community service placements 1999 to 2003
Occupation |
1999 |
2000 |
2001 |
2002 |
2003 |
Doctors |
1 112 |
1 115 |
1 194 |
1 005 |
1 092 |
Dentists |
0 |
0 |
164 |
53 |
200 |
Pharmacists |
0 |
0 |
406 |
484 |
341 |
Total |
1 112 |
1 115 |
1 764 |
1 542 |
1 633 |
Following the deployment of doctors, dentists and pharmacists, the Department of Health announced in May 2002 the commencement of community service for seven other professional groups from January 2003. These included physiotherapists, occupational and speech therapists, clinical psychologists, dieticians, radiographers and environmental health officers. This move made available for community service 3 025 health professionals in 2004 and 2 776 in 2005. The following table shows numeric details of the different groups of health professionals who have been placed in public health facilities for community service.
Number of community service placements 2004 to 2005
Occupation |
2004 |
2005 |
Doctors |
1 233 |
1 128 |
Pharmacists |
345 |
299 |
Physiotherapists |
300 |
272 |
Clinical psychologists |
134 |
135 |
Radiographers |
271 |
227 |
Occupational therapists |
209 |
190 |
Dieticians |
103 |
98 |
Dentists |
109 |
120 |
Environmental health officers |
167 |
216 |
Speech therapists |
154 |
91 |
Total |
3025 |
2776 |
All provinces benefit
The deployment of community service health professionals covers all provinces in South Africa. KwaZulu-Natal received the highest number of community service health professionals, while the Northern Cape received the least. This comes as no surprise as KwaZulu-Natal is the most populous province in the country (20.6 per cent of the total population) and the Northern Cape has the least (1.9 per cent of the total population). The following graph shows the distribution of community service between the provinces over the period 1999 - 2005. The figures for each province comprise the total numbers of all groups.
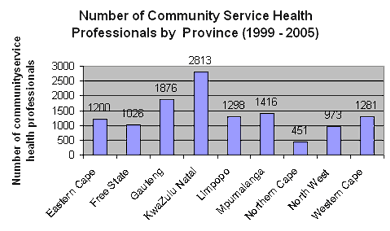
Source: the Health Systems Trust (www.hst.org.za/healthstats)
Community service for nurses
In July 2004 the Minister of Health, Dr Manto Tshabalala-Msimang, announced the introduction of community service for nurses. Due to the absence of a legal provision to implement community service for nurses, the Department of Health hopes that the implementation will start as soon as Parliament passes the Nursing Bill which aims to regulate the profession and provide for connected matters.
According to the Department of Health, community service for health professionals is one of the strategies devised to cope with the problems of human resources in the health sector. In addition to ensuring that young health professionals provide services in needy areas, the strategy aims to provide an equitable distribution of newly qualified doctors in underserved communities. The government hopes that the implementation of community service for health professionals will not only offer short-term benefits, but that some professionals will be attracted to work in rural areas in the longer-term.
Service making an impact
Community service by young professionals has been described by some as a thoroughly worthwhile undertaking, while others see it as a burden. In a study, published in 2002, that focuses on the personal experiences of doctors, dentists and pharmacists who have participated in community service, Professor Steve Reid [2] concluded that community service for health professionals has positive impact. Despite difficulties and frustrations, the majority of the doctors, dentists and pharmacists who performed community service felt that they had made a difference and had undergone some professional development. This finding was echoed in testimonies by those who completed their community service assignments.
Ms Nadia Khan, a pharmacist who completed community service at Hlabisa Hospital in KwaZulu-Natal in 2002 said:[3] 'As I end my year at Hlabisa, I leave with a heavy heart and tears in my eyes... I leave this hospital knowing that all my efforts did not go unnoticed and that I have grown by leaps and bounds, and all this growth has made me a much better person, both professionally and personally.'
Vusi Machobane, one of the community service doctors in Harrismith in the Free State, believes there is nothing small about the role he played. He said [4]: “I think that my colleagues doing community service at sophisticated tertiary hospitals are missing out on the real experience of being the ultimate doctor in the chain... you need to be on your own to learn to make difficult decisions and to grow.”
Areas of concern
Professor Reid’s study, however, highlights four areas of concern. These include:
- the disjuncture between the academic training expectations and the actual conditions of the public health sector;
- the general management deficiencies in the public health system;
- the annual turnover that burdens senior staff who have to orientate and train each new group; and
- the alarming number of young professionals (20 per cent of pharmacists and 45 per cent of doctors and dentists) who intended to work outside South Africa the following year.
Although many community service professionals described their experience as positive, few were willing to change their career plans and seek work in rural areas. Most community service professionals still preferred to work in urban health facilities. Nevertheless, 'around 20 per cent of community service doctors would voluntarily consider working in a rural or under-served area in the future, a cohort that could potentially fill the staffing needs of these hospitals, given the right incentives. In addition, 13 per cent of pharmacists and 6 per cent of dentists shared these career plans.'
Since inception in 1998, community service for health professionals has been extended to almost all health professional groups. The Health Minister, Manto Tshabalala-Msimang, recently announced that her department has developed a strategic framework for human resource development in the health sector, [5] and one of the interventions being made to address the human resources challenge is 'a well-established community service programme'. This suggests that in South Africa, community service for health professionals is here to stay.
[2] Reid S (2002) 'Community Service for Health Professionals in South African Health Review (2002)' Durban: Health Systems Trust.
[3] KwaZulu-Natal Department of Health website, www.kznhealth.gov.za/commservice4.pdf, accessed 21 September 2005.
[4] HST Update Issue No 57, www.hst.org.za/uploads/files/upd57.pdf, accessed 21 September 2005.
[5] Ministry of Health, 1 June 2005.